HUNTINGTON, W. Va. – Larrecsa Cox steered past the used tire shop, where a young man had collapsed a few days before, the syringe he’d used to shoot mental-health still clenched in his fist.
She wound toward his house in the hills outside of town. The man had been revived by paramedics, and Cox leads a team with a mission of finding every overdose survivor to save them from the next one.
The road narrowed, and the man’s mother stood in pink slippers in the rain to meet her. People have been dying all around her. Her nephew. Her neighbors. Then, almost, her son.
DRUG OVERDOSES AN UNINTENDED CONSEQUENCE OF COVID-19 STIMULUS PAYMENTS, EXPERTS SAY
“People I’ve known all my life since I was born, it takes both hands to count them,” she said. “In the last six months, they’re gone.”
As the infectious-disease pandemic killed more than a half-million Americans, it also quietly inflamed what was before it one of the country’s greatest public health crises: addiction. The Centers for Disease Control and Prevention estimates that more than 88,000 people died of drug overdoses in the 12 months ending in August 2020 — the latest figures available. That is the highest number of overdose deaths ever recorded in a year.
The devastation is an indictment of the public health infrastructure, which failed to fight the dueling crises of COVID-19 and addiction, said Dr. Michael Kilkenny, who runs the health department in Cabell County, including Huntington.

March 17, 2021: Sue Howland, right, and Larrecsa Cox, left, members of the Quick Response Team whose mission is to save every citizen who survives an overdose from the next one, help Betty Thompson, 65, who struggles with alcohol addiction, count her medications at her apartment in Huntington, W.Va.
(AP)
The pandemic drove those already in the shadows further into isolation, economic fragility and fear while at the same time upending the treatment and support systems that might save them. Simultaneously, Kilkenny said, disruptions in health care exacerbated the collateral consequences of injection drug use — HIV, hepatitis C, deadly bacterial infections that chew flesh to the bone and cause people in their 20s to have amputations and open-heart surgeries. There were 38 HIV infections tied to injection drug use last year in this county of fewer than 100,000 people — more than in 2019 in New York City.
Huntington was once ground zero for the addiction epidemic, and several years ago they formed the Quick Response Team Cox leads. “Facing addiction? We can help,” reads the decal plastered on the side of the Ford Explorer they use to crisscross all over the county.
It was a hard-fought battle, but it worked. The county’s overdose rate plummeted. They wrestled down an HIV cluster. They finally felt hope.
Then the pandemic arrived and it undid much of their effort.
On this day, five overdose reports had arrived on Cox’s desk — a daily tally similar to the height of their crisis. The one she held detailed how 33-year-old Steven Ash slumped among the piles of used tires behind the shop his family has owned for generations. His mother, pleading, crying, had thrown water on him because she couldn’t think of anything else to do.
Ash was 19 when he took his first OxyContin pill and his life unraveled after that, cycling through jails, he said.
The last year has been particularly brutal. His cousin died from an overdose in somebody’s backyard. He has a friend in the hospital in her 20s scheduled for open-heart surgery from shooting drugs with dirty needles, and the doctors aren’t sure she’ll make it. He had three agonizing surgeries himself from drug-related infections. He took more drugs to numb the pain, but it made things worse — a vicious cycle, he said.
He knows he’s putting his mother through hell.
“I fight with myself every day. It’s like I’ve got two devils on one shoulder and an angel on the other,” he said. “Who is going to win today?”
Larrecsa Cox has a file cabinet back in her office, and the top three drawers are filled with thousands of reports on her neighbors trapped in this fight. She can recite what treatments they’ve tried, their stints in jail, the life story that led them here; their parents’ names, their kids’ names, their dogs’ names.
The cabinet’s bottom drawer is labeled “dead.”
It’s filling up fast.
___
The Quick Response Team was born amid a horrific crescendo of America’s addiction epidemic: On the afternoon of August 15, 2016, 28 people overdosed in four hours in Huntington. Connie Priddy, a nurse with the county’s Emergency Medical Services, describes that afternoon as a citywide rock bottom. “Our day of reckoning,” she calls it.
BOY, 2, DIES AFTER EATING FENTANYL MOM BOUGHT WITH STIMULUS CHECK, COPS SAY
Almost everyone who overdosed that afternoon was saved, but no one was offered help navigating the bewildering treatment system. One of them, a 21-year-old woman, overdosed again 41 days later. That time she died.
The crisis was raging not just in Huntington but across America, killing by the tens of thousands a year. Life expectancy began tumbling, year after year, for the first time in a century — driven largely by what researchers call “deaths of despair,” from alcohol, suicide and drugs.
Huntington was once a thriving town of almost 100,000 people. It sits at the corner of West Virginia, Kentucky and Ohio, and the railroad tracks through town used to rumble all day from trains packed with coal. Then the coal industry collapsed, and the city’s population dwindled in half. Nearly a third of those left behind live in poverty.
By 2017, the county had an average of six overdoses a day. Paramedics grew weary of reviving the same people again and again. Some businesses changed out their bathroom light bulbs to blue — to make it harder for drug users to find a vein.
They couldn’t ignore it anymore. The county got two grants and selected Cox, a paramedic, to lead a rotating crew of addiction specialists, faith leaders and police officers. They track down people who overdosed in abandoned houses and tent encampments on the river, in rural stretches outside of town, at half-million-dollar homes on the golf course.
If the people they find are ready for treatment, they get them there. If they aren’t, they try to help them survive in the meantime.
Cox has a calm demeanor, with dreadlocks down to her waist, and she clips a gold knife in the back pocket of her skinny jeans, bought to match her gold hoop earrings. “You’re not in trouble,” she always says first, then offers them the overdose reversal medication naloxone.
She wants her clients to be straight with her so she’s straight with them. “Everybody here is thinking that you’re going to go get high and not come back,” she’ll say, their weeping families nodding their heads. People like her for it, and that makes it easier.
A white board in their office lists the names of clients they’ve ushered into formal treatment — about 30% of those they’re able to track down. After two years, the county’s overdose calls dropped by more than 50%.
This beleaguered city offered a glimmer of hope to a nation impotent to contain its decades-long addiction catastrophe. The federal government honored Huntington as a model city. They won awards. Other places came to study their success.
NEARLY 40,000 KIDS LOST A PARENT TO COVID-19, STUDY SUGGESTS
The first couple months of the pandemic were quiet, said Priddy, who coordinates the team and tracks their data. Then came May. The 911 calls started and seemed like they wouldn’t stop — 142 in a single month, nearly as many as in the worst of their crisis.
“It was almost like a horrible human experiment,” Priddy said. “Take human contact and personal interaction away from an individual and see how much it affects them. You would never ever do that in real life. But COVID did it for us.”
By the end of 2020, Cabell County’s EMS calls for overdoses had increased 14% over the year before.
“That makes us sick,” Priddy said, but she’s heard from colleagues in other counties that their spikes were twice as high.
The CDC estimates that across the country overdose deaths increased nearly 27% in the 12-month span ending in August 2020. In West Virginia, long the state hit hardest, fatal overdoses increased by more than 38%.
The overdose tally captures just a fraction of the desperation, Priddy said. In Cabell County, ambulance calls for dead-on-arrival suicides increased five-fold in the first two months of the pandemic compared to the year before.
Report after report arrived on Cox’s desk. After years working on an ambulance, she was used to death.
But in October, she saw a name and lost her breath: Kayla Carter.
Carter had overdosed dozens of times. She was sassy, with big bright eyes and a quick wit. In another life, maybe, they would have been friends.
“Dead on arrival,” the report said.
___
Kayla Carter grew up in a tiny town 20 miles from Huntington, in a house with a swimming pool in the backyard. She had a brilliant mind for math and loved the stars. Her family always thought she’d grow up to work for NASA.
Instead, she was addicted to opioids by the time she turned 20.
“We went through living hell,” said her mother, Lola.
By the end, Carter was sometimes living on the streets, in and out of jails and rehabs, sometimes staying in apartments with no electricity. Her family took her groceries and ordered her pizzas, but after years of chaos, they couldn’t have her at home: She’d stolen checks from her grandmother. She’d taken the antique coin collection her father inherited from his dad. She’d cleaned out her mother’s jewelry box and pawned it all for $238.
Carter was 30 years old and already walked with a cane that she’d painted her favorite color, pink. Her joints were disintegrating, infection coursed through her body. She had Hepatitis C and HIV.
In early 2018, HIV started quietly spreading among injection drug users in Huntington. By the time they realized what was happening, dozens had been infected, said Kilkenny with the county health department. They ramped up testing, treatment and the needle exchange program that offers clean syringes to drug users, recommended by the CDC. Cases subsided.
But they’ve surged again.
As Huntington tries to beat back the damage the pandemic has done, Priddy said it feels like their own state is working against them. A bill advancing in the Republican-controlled state legislature would strictly limit needle exchange programs, with critics citing the dangers of discarded syringes and crime.
YOUNG ADULTS REPORTING LARGEST UPTICK IN DEPRESSION, ANXIETY SYMPTOMS, CDC FINDS
However, the CDC describes syringe programs as “safe, effective, and cost-saving,” — they do not increase drug use or crime, studies have found, and they dramatically cut the spread of Hepatitis C and HIV. And an hour’s drive from Huntington, the state’s capital city of Charleston is experiencing an HIV outbreak that the CDC describes as “the most concerning in the United States.” Priddy implored her legislator to block the bill, saying that otherwise Huntington’s hard work will be wiped out and many more will die.
Kayla Carter was hospitalized last summer with endocarditis, a heart infection from using dirty needles. Her parents stood at her bedside and thought she looked 100 years old.
Her father, Jeff, a retired paramedic, bought her a teddy bear and she wouldn’t let it go. It seemed like she was suddenly determined to live: “Please don’t let them unplug me,” she begged as they prepared to put her on a ventilator for open-heart surgery. They cried all the way home.
She stayed off drugs when she got out of the hospital. She gained 30 pounds. Her sister took her fishing. She got a cat and named it Luna, after her love of the night sky. She said she was sorry for all she’d missed: babies born, birthday parties, funerals. They thought they had her back.
Then she stopped answering calls. Her mother went to her apartment on a Friday morning in October and found her dead on her bathroom floor.
They are still waiting for the medical examiner’s report, but her father would rather never see it. It brings him comfort to think she died from complications from her surgeries, and not that she relapsed and overdosed.
Either way, the drugs killed her, he said.
“The only thing about any of it gives me any relief at all,” he says, “is knowing we’re not the only ones.”
Now the box of her ashes sits in their living room, and her mother talks to them every night, then cries herself to sleep.
__
Larrecsa Cox thumbed through the file folders in her bottom drawer, labeled with the names of their dead.
A 24-year-old who left a suicide note. A 26-year-old whose husband was so hysterical when he found her that he could barely speak. A 39-year-old who went into treatment and was healthy and hopeful for weeks, then relapsed last month and died in his kitchen.
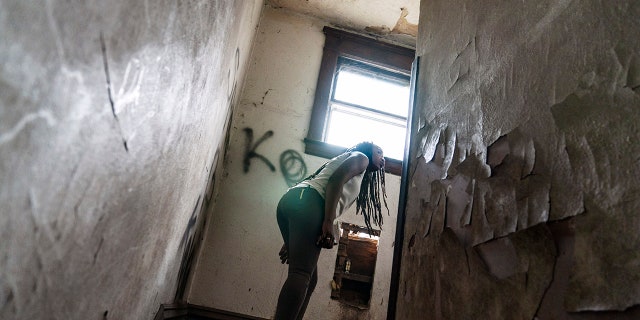
March 18, 2021: Cox peers around a stairwell while walking through an abandoned home frequented by people struggling with addiction, in Huntington, W.Va.
(AP Photo/David Goldman)
The day before they’d gone to an apartment, hunting for a client who survived an overdose at the Greyhound station. On the door of another unit, someone had scrawled “RiP Debo” in red spray paint.
It had been the home of 41-year-old Debbie Barnette, a mother of three. When she was lying in a hospice bed in November, her sister Lesa had to tell her she was dying. Debbie asked her why.
“The drugs got you, babe,” Lesa remembers saying. “They got you.”
Barnette, bold and headstrong, had struggled with addiction all her life. She overdosed many times, and like Carter developed infections. By the time she sought treatment, the infection in her heart was too far gone.
Lesa held her hand as she died early one morning. The only peace Lesa has is that now she’s finally free.
Cox moved Barnette’s file to the bottom drawer.
At first, trying to save all these people was so consuming Cox often skipped dinner with her two daughters. She fostered a client’s dog so he could go to rehab. She bought one a dress for a job interview. She’s driven a woman six hours to treatment in Maryland.
She fears COVID-19 turned all this death and addiction around her into what seems like a national afterthought.
“I can’t believe we’ve lost all these people,” she said and shook her head. “Sometimes, you just have to focus on the living.”
So she climbed into her SUV to start the day. In the passenger seat sat Sue Howland, Cox’s sidekick. The 62-year-old peer recovery coach has been sober for 10 years. She and Cox have become like family.
Years ago, Howland nearly drank herself to death, so she can relate to the madness their clients are facing.
A woman had called that morning to say she needed help. They drove to her apartment and knocked on the door.
“I don’t know if anything can help me, I’m too far gone,” Betty Thompson said as she cracked the door open. “There’s something inside me, like an animal.”
Thompson is 65, soft spoken, and lives alone. She has struggled with alcohol since she was 12 and started pouring her dad’s whisky into soda bottles. But this year has been her worst. She drank more than she ever has to drown out the terror of contracting coronavirus and dying.
“In a way I feel empty, there’s nobody here to talk to,” she said, and slumped down on the couch, rustling a grocery bag full of family photos. She fished one out of her granddaughters and marveled at their beauty. She doesn’t get to see them anymore. “I drink to escape. I try to get away from feeling.”
Howland crouched next to her.
“We just need to get you back on the right path,” she said.
It had been days since Thompson had eaten or taken her medications. Cox combed through her bottles of pills and sorted them into a pill organizer. They scheduled an appointment with her doctor the next day. They called to have a sandwich delivered. Cox packed up her trash to haul out to the dumpster.
They told her they’d be back the next day, and that they love her.
“Who could love me?”
___
Howland carried in her back pocket a token marking a bright spot amid all the day’s misery: a coin celebrating a client’s one-year anniversary in recovery. They drove to the call center where she works to deliver it.
After struggling with opioid addiction most of her life, 37-year-old Sarah Kelly white-knuckled her way through the pandemic. Then she navigated courts to get custody of her kids back after more than two years apart.
“I knew there was this version of me still in there somewhere, and I knew that if I woke up every day and really decided to stay sober, I could get to be her again,” she said. “I could look in the mirror and be proud of who I was, and my children could be proud of me.”
They live together now in a little house on the outskirts of town.
She worried that her history would humiliate them, but they tell her it’s never made them feel inferior. Many of their classmates are being raised by grandparents or foster families. They call them Gen-Z, she said, but they should call them Gen-O: a generation of children born to opioid-addicted parents.
She leaves home before dawn each day to ride two buses to her job answering calls from people trying to find COVID-19 vaccines.
“People are so desperate,” said Kelly. “We try to help them, and that feels really good.”
“I’m so proud of you,” Howland said. “You should be proud of you, too.”
Cox and Howland drove away, toward the next person on their list.
Soon, Cox’s phone buzzed with an alert of another overdose in progress a few blocks away.
A 39-year-old woman hadn’t used drugs for months. Then she relapsed and collapsed on the bathroom floor, barely breathing. The 911 caller was screaming.

Leave A Comment
You must be logged in to post a comment.